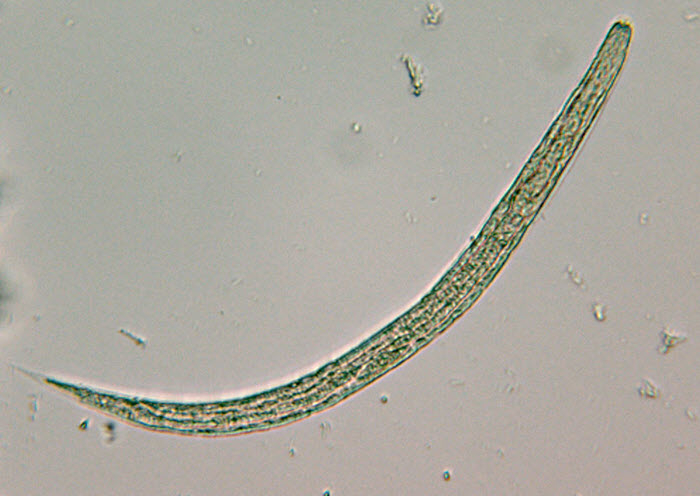
Strongyloidiasis is a disease caused by parasitic nematodes (round worms) belonging to the genera Strongyloides. Even as adults these round worms are very small – no longer than 1.5 mm.
Risk areas
Strongyloidiasis is especially associated with tropical and subtropical parts of the world, but you can catch the disease anywhere in the world if you’re unlucky since the parasite can spread directly from one person to the other without needing any intermediary host that would limit its geographical range. There are for instance numerous examples of how military staff infected in South East Asia have spread strongyloidiasis within the United States after returning home from active duty.
Transmission
Soil
The most common transmission route is through soil containing free living parasites.
You don’t need to ingest the soil or get it on a mucous membrane to get infected – the parasites can pierce through intact skin. Walking barefoot or doing gardening chores without gloves can be enough.
Human to human
Direct infection from human to human is possible. The nematodes present in the faeces of an infected human is ready to infect another human right away; no other animal is needed as an intermediary host.
Human to human transmission of Strongyloides nematodes is associated with environments where people are in close contact with each other and strict personal hygiene routines may be lacking. Human to human transmission have for instance been reported from daycare centres (for children), care facilities and special facilities for people with impaired cognitive skills.
Organ transplant
Strongyloides nematodes can be transmitted through organ transplant if the donor is infected.
Symptoms
A person with a strong immune system and no underlying health problems will often notice no symptoms or only mild symptoms when infected with Strongyloides nematodes. There are plenty of examples of people who got infected a long time ago and then unknowingly carried the nematodes inside for years or even decades until something else weakened the body’s immune system and the nematodes began causing symptoms.
Strongolydiasis symptoms
Entry stage: When the nematodes pierce through the skin, they can cause localized skin irritation.
A few days after the infection date: Symptoms from the respiratory tract can manifest a few days after the infection date. If the parasites cause fatigue and a dry cough, it is called Löffler’s syndrome.
Approximately two weeks after the infection date: This is when you might start noticing symptoms from the digestive tract, such as heart burn, stomach pain and gassiness. Some people develop alternating constipation and diarrhoea.
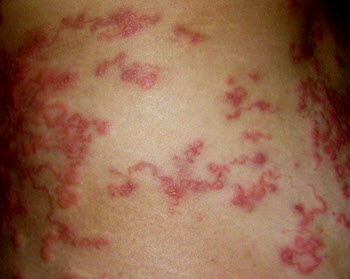
Migratory stage: As parasites in their larval stage start migrating throughout the body you may develop skin problems, such as hives. A red rash on the buttocks and around the waist is another tell-tale sign.
Symptoms from the respiratory tract and digestive tract can manifest together with the skin problems. None of the three symptom groups are mutually exclusive.
Hyper infection syndromes
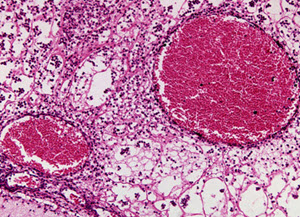
 Hyper infection syndrome is a very serious condition brought on by nematodes piercing through the intestinal wall and entering the host’s cardiovascular system. Hyper infection syndrome, which is typically seen only in persons with a severely impaired immune system, can be lethal.
Hyper infection syndrome is a very serious condition brought on by nematodes piercing through the intestinal wall and entering the host’s cardiovascular system. Hyper infection syndrome, which is typically seen only in persons with a severely impaired immune system, can be lethal.
The parasites aren’t just dangerous in themselves; their piercing through the intestinal wall will also make it possible for intestinal bacteria to enter the cardiovascular system. Through the cardiovascular system, the bacteria will reach various parts of the body where they can cause infections, e.g. meningitis.
As mentioned above, strongyloidiasis hyper infection syndrome is typically only seen in patients with a weakened immune system. This can be caused by various underlying problems, such as HIV infection, serious malnutrition, radiation sickness, late stage tuberculosis, late stage syphilis, aplastic anaemia, or immune-suppressive treatment (e.g. after an organ transplant).
In countries where strongyloidiasis is fairly common, many hospitals will routinely test the patient for strongyloidiasis before administering immune-suppressive treatment.
Confirming the diagnosis
Blood, faeces and/or duodenal fluid can need to be analysed when strongyloidiasis is suspected.
Checking the faeces only is perilous, since a person can be infected without excreting parasites in their stool.
Blood can be tested for antibodies against Strongyloides parasites, but it can be difficult to tell such antibodies apart from antibodies created against closely related parasites. Also, it is impossible to know if the presence of antibodies indicate a current infection or if they just remain from a previous infection. Important: A person with an impaired immune system can be infected with Strongyloides parasites without developing antibodies.
In some countries, specialized laboratories will do parasite cultures when strongyloidiasis is suspected. One such lab is found within the School of Tropical Medicine in London.
Treatment
The parasites are sensitive to several different anti-parasite medications, including common medicines such as ivermectin, thiabendazole and albendazole.
Ivermectin is a common treatment choice and is very efficient in killing adult parasites. Typically, at least two treatment rounds are necessary. You want to make sure that all parasites that were juvenile during the previous treatment round are killed.
It is important to carry out all treatment rounds even if your symptoms disappear after the first round. Vanishing symptoms doesn’t automatically mean that all the parasites are dead.
Life cycle
- The parasites enter the host’s body, e.g. by piercing through the soles of the feet when a person is walking barefoot in soil infested with parasites.
- Inside the host, the parasites migrate to the small intestine where they burrow and deposit their eggs.
- The eggs hatches in the host’s small intestine and round worms emerge.
- A majority of these round worms will leave the host when the host defecates. Some will stay however – they burrow into the intestinal wall to avoid being expunged. The round worms that stay will lay new eggs, completing their life cycle within the host where they themselves were hatched. This is known as auto-infection.
- The round worms that left with the faeces are ready to find a new host and start the life cycle over again in that host.